|
|
Functional Electrical Stimulation Field
Converges in Cleveland
by James Cavuoto, editor
The spirit of a new industry and the promise of groundbreaking medical
technology was in the air in Cleveland at the sixth annual conference
of the International Functional Electrical Stimulation Society meeting
in June. The five-day event, themed “Envisioning a New Century
of Breakthroughs,” highlighted six "millennium" papers on key
areas of neurotechnology, a truly international assembly of presenters,
a small but solid core of neurotech manufacturers and sponsors,
and several unique attributes not often found at a scientific or
engineering meeting. A ubiquitous spirit of interdisciplinary cooperation
linked this assemblage of biomedical engineers, neuroscientists,
clinicians, therapists, and funding agencies. Several vividly interactive
sessions featured frank, if at times cutting, discussion of research
and product directions. A team of spinal cord injury patients was
on hand—not just as poster children—but as active participants
offering feedback and product suggestions to the engineers in attendance.
 |
|
| A panel of Spinal cord
injury patients offered attendees critical feedback on current
devices and future directions. |
|
In a gripping keynote address, neurosurgeon
and deep-brain stimulation pioneer Andres Lozano from the University
of Toronto presented an overview of the use of DBS systems for treating
neurological disorders such as Parkinsons, stroke, and tremors.
Lozano related some impressive results treating serious cases with
implanted electrodes in subcortical nuclei in the brain. He expects
that neurodegenerative disorders will overtake cancer as the number
two killer by 2040, when approximately one-third of the population
will be affected. Looking beyond medical therapeutics, Lozano sees
a coming merging of mind and machine as computational power increases
and device miniaturization continues to create systems that rival
the brain's connective population of 10^15
synapses and 1 millisecond time scale. He mentioned the possibility
of someone acquiring preformed neural circuits that would endow
the recipient with vital knowledge bases or motor skills. He also
believes brain stimulation may have far-reaching applications treating
obesity, depression, and other conditions.
Regeneration
One of the most productive sessions at the conference was a workshop
devoted to neural repair and functional restoration. It highlighted
several strategies for combining stimulation with neurobiological
means of regenerating and repairing neural tissue. Researchers have
found that an electric field oriented in the direction of a damaged
neural fiber can enhance axonal regrowth. Panelists also discussed
efforts underway to build hybrid neural/silicon devices that can
be implanted in the nervous system to improve communication between
artificial devices and neural centers. Entirely new or rebuilt pathways
can be constructed in the nervous system by using stimulation to
direct neurons and neurites to migrate and connect in the desired
locations.
In another example of interdisciplinary cooperation, IFESS, composed
largely of biomedical engineers, aligned with an association of
surgeons and clinicians to coproduce a new journal called Neuromodulation.
Control and Engineering
Several sessions at the conference looked at progress in improving
first-generation neural prostheses for hand grasp, bladder control,
and standing/walking systems. Attendees argued for more natural
human interfaces in the devices. For example, instead of the shoulder-actuated
control currently used in many hand-grasp prostheses, a system controlled
using electromyographic signals from the arm muscles, or a sensor
that is based on the user's wrist angle, is felt to be more natural.
In the bladder control stimulator market, current products such
as NeuroControl's VoCare system work only by performing a surgical
procedure known as rhizotomy, which deprives male patients of sexual
function. New products that no longer require the rhizotomy are
under development at a number of research institutions.
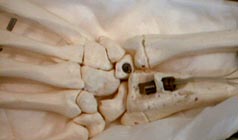 |
This surgically
implanted wrist-angle sensor developed at the Cleveland FES
Center offers a more natural user interface to a hand-grasp
prosthesis. |
Development of lower-extremity neural prostheses
for standing and walking was the subject of pointed discussion during
many sessions. Control engineers trying to perfect closed-loop feedback
electronics that enable paralyzed patients to walk clamored for
better sensors that offer precise information on biomechanical properties
such as limb position and muscle force. Some neural engineers dismissed
the overdependence on control theory as "mental masturbation." One
participant, Gerald Loeb from the University of Southern California,
claimed that efforts to build a walking prosthesis over the last
20 years have been misguided and the resources could have been directed
to more achievable problems. Nonetheless, progress to date on standing
and walking prostheses has many paraplegic patients and clinicians
understandably excited, and the problems that remain appear to engineering
issues and not limitations of basic science.
Consensus
Participants agreed that progress in smaller and smarter microelectrodes,
including electrodes with multiple contact points and electrodes
coated with neurophilic substances that promote electrode/neuron
interaction, will be a key factor in the development of future products.
There was also general agreement that the timing and sequence of
patterned muscular activity after a spinal cord injury, stroke,
or other neurological incident is critical to the patient's prospects
for regaining function. Passive muscle stimulation and exercise
patterns of simulated walking in paralyzed patients not only help
counteract muscle atrophy and pressure sores, they also increase
the probability that the patient will regain either natural or artificial
use of the lost muscle function. Rahman Davoodi from USC showed
a rowing machine for paraplegics that uses electrical stimulation
to direct the sequenced activity of leg motions. This type of product
appears to have considerable commercial potential for rehabilitation
centers and even in-home use.
Government representatives on hand included Michael Weinrich, director
of the NIH's National Center for Medical Rehabilitation Research,
William Heetderks, of the National Institute of Neurological Disorders
and Stroke, and Laura Bowman of the Department of Veterans Affairs.
The two NIH organizations are the largest U.S. government funders
of neural engineering programs, about $50 million per year--an amount
that seem paltry given the promise of this technology. Weinrich
said that the newly established National Institute of Biomedical
Imaging and Bioengineering would have a budget of about $40 million
in new funds, not counting funds diverted from existing institutes.
Researchers in this field are nervously watching developments at
the new institute. Some are optimistic that neural engineering can
get a foothold in the new funding source; others are worried that
key researchers and existing funds will be diverted from NINDS and
NCMRR or that medical imaging will dominate at NIBIB.
Vendors
Exhibitors and sponsors at the event included several of the early
manufacturers of neurotechnology products and systems. NeuroControl
Corp. showed its FreeHand hand grasp proesthesis, the VoCare
bladder stimulation system, and a new miniaturized multi-channel
programmable stimulator call StIM. The device is targeted at stroke
patients suffering from shoulder pain caused by the separation of
the shoulder joint and weak muscles after stroke.
Medtronic, probably the largest
corporation in the business—even though its neurotechnology
product line is dwarfed by its cardiac products—promoted its
InterStim urinary control system and DBS product line.
Cleveland Medical Devices
showed its BioRadio 110, a compact and wireless brain monitoring
device. Besides EEG signals, the product can transmit sensed ECG,
EMG, EOG, and PSG signals to a nearby PC-based monitor. EIC
Laboratories in Massachusetts exhibited its range of electrode
coating products and services, which work with gold, platinum, silicon,
iridium, and other materials. Empi
showed its line of stimulators for pain treatment and neuromuscular
rehabilitation. NeuroStream
Technologies, a Canadian manufacurer, showed its line of implantable
NeuroCuff interfaces, which accommodate electrodes as well as catheters
for fluid infusion. Neopraxis
Pty Ltd., an Australian firm, promoted its 22-channel Praxis
stimulator, targeted at paraplegic patients. Advanced
Bionics, one of the leaders of the cochlear implant business,
promoted its line of BION leadless stimulators. The compact devices,
measuring 16 mm long by 2 mm in diameter, can be inserted in a patient
with a 12-gauge needle and controlled by a wearable RF transmitter.
In an intriguing prelude to the conference, nearby Case
Western Reserve University, home of many of the pioneers of
functional electrical stimulation, sponsored an Applied Neural Control
Research Day, which updated attendees on developments in neuromuscular
stimulation, electrode design, and other emerging technologies.
The Cleveland FES Center,
which organized the conference, had a large contingent of researchers,
presenters, and technicians on hand. The non-profit organization
is funded by the VA, CWRU, and MetroHealth Medical Center, and helps
design neural prostheses which are later spun off to private industry.
Southern California was also well represented at the event. Besides
the team from Advanced Bionics, the newly established Alfred
E. Mann Foundation, as well as related teams from USC, the Alfred
Mann Institute, and visual prosthesis company Second
Sight llc were on hand.
|
|


